The clinic is four minutes from my house – at least that was what Google maps said. Turn a right, another right, then a left and it’s on the right.
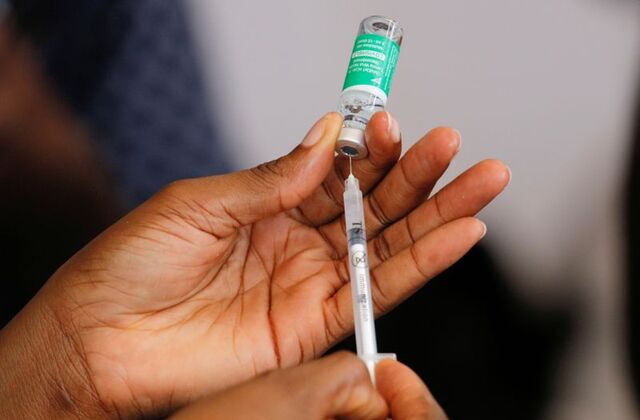
Like all the previous ones I’ve seen, the Corona Virus Disease (COVID-19) wing of the clinic is a big white tent at the edge of the land; I like to think it is a silent prayer that the pandemic would be over soon. The doctor I had booked my vaccine appointment with is standing outside the tent; she is wearing blue scrubs and seems to be middle-aged. “They didn’t let you drive in?” she asks as I walk towards her. “No,” I reply, and after exchanging pleasantries, she ushers me inside, and I take a seat. Inside, the tent is divided into two; separated by a table, the smaller half is used as a reception/admin while doctors sit at the other side – educating patients about the vaccine (side effects, etc.), administering the vaccine, and spending their free time chatting among themselves.
“I’m here for my second dose,” I say, after greeting the office, even though I already explained it to the doctor on the phone a few days earlier. I hand over my green vaccine card, and even before being asked, I start to explain: “I had my first dose in May and was supposed to get the second one done in July.” This is the last week of November. I watch the doctors pass the vaccine card among themselves, quite unsure of what to do next. They spend a few moments contemplating calling someone – perhaps a more experienced doctor or the hospital – to ask about my case but then decide to proceed anyway. Looking at their puzzled faces, I begin to narrate how I got ill after getting my first vaccine shot; not only was my left arm sore for days, but I also ran a fever, had a terrible constant headache, muscle ache, and was exhausted and nauseated for three days. It was like having Malaria and typhoid at the same time in a foreign country with no anti-malaria drug available – you have no idea how to treat it or when it will go; it’s just vibes and insha Allah and perhaps a few drops of the Blood of Jesus. I didn’t want to go through that; I have a full-time job, and I could not afford to be ill.
“AstraZeneca, right?” a male doctor asks. I nod yes, and he brings out the vaccine bottle, passes it to me to read the label before piercing the bottle with an injection. I flinch as he gets closer, holding my left arm with my right hand. My fear of injection aside, this shot reminds me of the pain I went through after the first shot. I can’t relive that again. More importantly, not getting the vaccine means two things: 1) the possibility of getting COVID-19 again (a chance I am personally not willing to take) and 2) the possibility of being unnecessarily stressed with several post-arrival COVID-19 home tests and a 10-day isolation period when travelling in December (another chance I am not willing to take). For these two reasons, I squeeze my eyes shut, take a deep breath, and agree to be vaccinated.
While I believe my four months of hesitation is justified, many people have refused to get vaccinated for one reason or the other. Last month, I published an article on the COVID-19 and the dilemma of vaccine equity in which I wrote: “The most widespread myth about the vaccine is infertility. It has also been assumed to have long-term effects, have an imbed tracking device, be unsafe because of how quickly it was developed, alter one’s DNA, and inject people with the virus it aims to protect from. In addition, Damagum reports that it is believed that people with underlying conditions, people who have had been infected with the virus, people with suppressed immune systems and pregnant or breastfeeding women should not get vaccinated. Luckily, the University of Missouri Health Care (MU Health Care) has answered most – if not all – of the questions and has addressed the concerns of many Africans. Unlike popular belief, the COVID-19 vaccine cannot infect people with coronavirus because it does not contain a live virus. While some clinical tries reported side effects, the vaccine has been proven to be completely effective and safe. Before being approved, the vaccines were put through the same intensive Food and Drug Administration (FDA) process as all other vaccines and had met all the safety standards of the administration. Lastly, MU Health Care informed that there’s an amino acid sequence that is shared between a placental protein and the spike protein found in Coronavirus, but the expert opinion is that it’s too short to cause infertility.”
Many organizations, healthcare professionals and individuals – such as the World Health Organization, UNICEF and University of Missouri Health Care – have taken it upon themselves to educate the public about COVID-19. But as of the first week of October, only a mere 2.3 percent of Nigerians (approximately 2.54 million people) had been fully vaccinated, and only about 4.7 percent of the public have received one dose of the vaccine. In my essay, I also wrote about the possibility that the lack of trust Nigerians – and perhaps Africans – have in their governments has further discouraged many citizens from getting their COVI-19 vaccine shots. I wrote: “Thinking back to women like Fatima Damagum’s hairstylist who may never get vaccinated, I don’t think it’s lack of sensitization holding them back.
I strongly believe that sometimes –irrespective of everyone’s effort to educate, and how affordable the vaccine is – the mistrust many Africans have in their government would not allow them to take heed. Like the hairstylist argued, why should we believe that a government who has inadvertently allowed hundreds of children being kidnapped in their classrooms, hundreds of travellers to be reported missing on their journey, hundreds of dead bodies found on inter-state expressways and hundreds of innocent protesters shot mercilessly at the hands of soldiers has our best interest at heart? There is absolutely no reason to.” Furthermore, many Africans have resorted to paying for the vaccine cards to facilitate their travelling experience while avoiding the horrific side effects of the vaccine.
While among a certain group of people, questions such as “have you gotten your vaccine?”, “When will you go for your second dose?” and “which vaccine shot did you get administered?” have become the order of the day; among a different group of people, it is as though the pandemic does not exist. From my observations, this has nothing to do with one’s socio-economic background; I have met people from all walks of life who “do not believe in the vaccine” for whatever reason. So, while it is easy to blame the COVID-19 vaccine apathy on lack of education or awareness, what is, in fact, closer to the truth is that people who are avoiding the virus are doing so of their own volition. They simply do not believe in the vaccine, and as passionately as we can disagree, we must respect this.